
Image: Shutterstock
The use of retinol while breastfeeding lacks extensive studies, so little is known about its safety in lactating mothers. Retinol and retinoids are a group of compounds that are usually found in several skincare products for acne, skin pigmentation problems, fine lines, and wrinkles. They are available in topical and oral forms (1). Retinol and retinoids (especially oral forms) have been found to be harmful during pregnancy. This forms the basis of its use with caution while breastfeeding (2). Read on as we discuss the various aspects of retinol and retinoids for dermatological use when breastfeeding.
What Is Retinol?
Retinol is a form of vitamin A, a fat-soluble vitamin (3). Vitamin A is the first vitamin to become an FDA-approved anti-wrinkle product. Vitamin A and its derivatives form the group known as retinoids, which are known to slow the skin-aging process primarily by increasing the production of keratinocytesiXCells that majorly compose the outer layer (epidermis) of the skin and secrete keratin protein , retaining skin hydration, and reducing the breakdown of collagen in the skin. Retinoids are used to treat skin issues such as acne, rosaceaiXAn inflammatory skin condition causing redness and rash, usually on the nose and cheeks , psoriasisiXAn autoimmune condition that causes raised, red, and scaly patches on the skin. It occurs when skin cells multiply at an abnormally fast pace , pyodermaiXRare condition that causes skin ulcerations , and ichthyosisiXA condition that makes the skin thick, dry (like fish scales), red, and itchy . Retinol shows its biological action after transforming into active metabolites such as retinoic acid. These compounds work via nuclear receptors that act at the DNA level (4).
Differences Between Retinol And Retinoids
Image: Shutterstock
Retinol and retinoids are often used interchangeably when it comes to dermatological products. However, they are not the same. Retinol is a form of vitamin A, while retinoids denote an umbrella term that includes vitamin A and the compounds structurally and functionally related to it. Retinoids refer to both natural, biologically active forms of vitamin A (retinol, retinal, and retinoic acid) and synthetic derivatives of retinol (etretinate, acitretin, and tazarotene) (4).
Can You Use Retinol When Breastfeeding?
There is insufficient scientific data to interpret whether retinol and retinoids are safe while breastfeeding. However, evidence indicates their adverse effects if taken during pregnancy. Vitamin A is normally present in breast milk and is likely to be secreted in it (5). It is unknown to what extent topical retinoids are secreted in breast milk, but it is expected to be a small amount (6). However, lactating women should use even topical retinoids only under medical supervision. When using topical retinoids during breastfeeding, it is advisable to avoid applying them on the nipple, areola, or large body surfaces. Mothers should wash their hands after application and prevent the baby’s skin from coming in direct contact with the treated areas (7) (8).
Image: Shutterstock
What Are The Risks Of Using Retinol When Breastfeeding?
Retinoids, especially oral, may cause congenital anomalies if taken early in pregnancy. They have been found to be associated with fetal retinoid syndrome, which may present as restricted growth, hydrocephalusiXExcessive fluid buildup in the brain cavities , microcephalyiXA condition where a newborn’s head is smaller compared to the rest of the body , learning difficulties, cleft palateiXA birth defect that causes a gap or split in the mouth’s palate (roof) , heart problems, and ear and eye abnormalities in some newborns (2) (9). Studies on breastfeeding infants are scarce and unlikely to be carried out on a large scale due to ethical reasons. So, the recommendation to exercise caution while using retinoids while breastfeeding is based on the reported adverse effects during pregnancy.
If baby skin comes in contact with topical retinoids, it may cause side effects such as itching or redness (10).
Safe Skincare Alternatives When Breastfeeding
Image: Shutterstock
It is not necessary to cease all skincare treatments during breastfeeding. Retinoids are primarily used for acne and psoriasis, and certain alternative treatments may provide comparable results and be used safely in nursing mothers. However, it is advisable to consult a board-certified dermatologist first. Alternatives include:
For acne treatment (11)
- Azelaic acid: It is used topically and has antioxidant, anti-inflammatory, and comedolyticiXAgents that can unclog skin pores or hair follicles clogged with oil, dead skin cells, and bacteria properties. Twice daily application up to a maximum strength of 20% may be considered safe during breastfeeding.
- Benzoyl peroxide: When applied topically, it shows antimicrobial and keratolytic properties and may be used in combination with antibiotics. Systemic absorption is minimal, and twice daily application of products containing 5% benzoyl peroxide may be considered safe.
- Sodium sulfacetamide: It is a topical antimicrobial agent that may be used when breastfeeding. The only exception is if the breastfeeding infant has glucose-6-phosphate dehydrogenase (G6PD) deficiency or hyperbilirubinemia, as it may increase the risk of infantile jaundice and kernicterus.
- Salicylic acid: Safe when used topically in small amounts and for a short duration.
- Glycolic acid and lactic acid peels: They have shown limited skin penetration and may be safely used.
- Topical antibiotics: Antibiotics that are considered safe when used topically include clindamycin, erythromycin, and metronidazole.
- Oral antibiotics: Oral antibiotics such as penicillins, cephalosporins, and some macrolides (erythromycin and azithromycin) may be taken on prescription during breastfeeding (12).
- Intralesional corticosteroids: They may be considered lactation-safe as a minimum amount of steroid is absorbed. Effective for acne cysts and inflammatory nodules.
For psoriasis treatment (13)
- Topical corticosteroids: Avoid application on or near the nipples.
- Calcipotriene: It is a synthetic derivative of vitamin D meant to be applied on the psoriasis-affected skin areas.
- Phototherapy: Narrowband UVB and broadband UVB phototherapy may be used when breastfeeding. It may be used for both acne and psoriasis. However, visiting the treatment center two or three times per week may not be convenient when you have a newborn to care for.
Image: Shutterstock
Other Skincare Ingredients You Should Avoid When Breastfeeding
Skincare ingredients that lactating women are advised to avoid are (11) (14):
- Topical antiandrogens, such as Clascoterone cream 1%, as the effects on lactation are unknown
- Oral hormonal therapies
- Both topical and oral tetracycline, co-trimoxazole, and fluoroquinolone antibiotics
- Methotrexate used to treat psoriasis is contraindicated while breastfeeding (15)
- Hydroquinone in skin-lightening products should be used after consulting a dermatologist (16)
- Skincare products that contain potentially harmful chemicals such as parabens, phthalates, and triclosan (17)
Image: Shutterstock
How Early Can You Start Using Retinol After Pregnancy?
Though topical retinol therapy is considered low-risk post-childbirth, it is advisable to resume treatment with such agents after you finish breastfeeding your baby (18).
1. Can I use hyaluronic acid with retinol when breastfeeding?
Hyaluronic acid alone is considered safe during breastfeeding (19). However, as retinol is not usually recommended, the combination is less likely to be used. It is best to consult a dermatologist before using any combinations for skin treatment when breastfeeding.
2. What if I accidentally use retinol when breastfeeding?
Accidental use of retinol while breastfeeding is not likely to be harmful for your baby, especially if a topical product has been used (18). Nevertheless, do inform your doctor and take their opinion.
3. Does retinol affect breast milk?
Retinol is a normal component of breast milk and may be secreted in it (5). However, retinol has not been reported to otherwise affect breast milk.
4. Can I use retinol serum when breastfeeding?
All retinol or retinoid-containing products should be used with caution and under the supervision of a board-certified dermatologist.
Retinol and its related products are largely available over-the-counter and also as prescribed medications. It is advisable to use such products under medical guidance while breastfeeding. Ensure that your baby does not come in contact with the treated skin areas if at all you are using such products. Treatment, especially with oral retinoids, is best to be postponed till breastfeeding is over. Safer alternatives to retinoids for treating skin conditions such as acne and psoriasis are available, but they also require a doctor’s approval. Make sure you carefully read the labels before procuring skincare products to avoid potentially harmful ingredients.
Infographic: Skincare Treatments Considered Safe For Lactating Women
Safer alternatives to retinoids may be used to treat skin conditions such as acne when nursing. It is advisable to consult a board-certified dermatologist if your problem is severe. Both medications and skincare procedures may be useful in addressing such skin issues. The infographic below enlists some such alternatives.
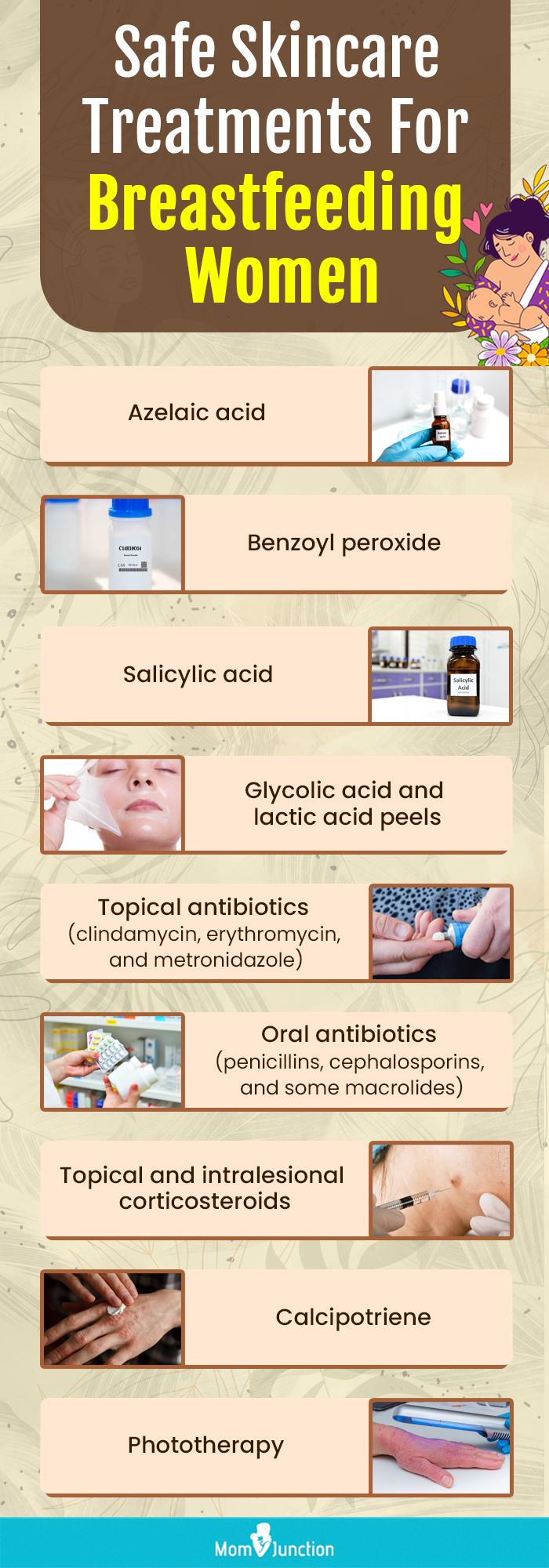
Illustration: Momjunction Design Team

Key Pointers
- Retinol may be present in several OTC skincare products.
- Retinol is a form of vitamin A, while retinoids comprise all compounds that are structurally and functionally similar to vitamin A.
- Retinoids are associated with adverse fetal outcomes and are usually not recommended during breastfeeding.
- Topical retinoids have less possibility to be present in breastmilk and may be considered low risk compared to oral ones.
- It is best to use alternatives such as glycolic acid and lactic acid peels wherever applicable.
